Pacemakers
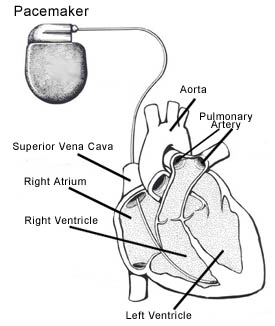 A pacemaker is an artificial device that electrically stimulates the heart's muscle to cause it to contract to initiate a heart beat. It is a small, lightweight electrical device surgically placed inside in the upper chest area. A pacemaker will make your heart beat more regularly. That will help ensure that enough oxygen and nourishment get to your body's cells. The device usually only works when it is triggered by an arrhythmia. A pacemaker may be temporary or permanent, depending on the patient's condition.
A pacemaker is an artificial device that electrically stimulates the heart's muscle to cause it to contract to initiate a heart beat. It is a small, lightweight electrical device surgically placed inside in the upper chest area. A pacemaker will make your heart beat more regularly. That will help ensure that enough oxygen and nourishment get to your body's cells. The device usually only works when it is triggered by an arrhythmia. A pacemaker may be temporary or permanent, depending on the patient's condition.
An artificial pacemaker system has two parts: a generator and wire (leads). The pacemaker generator is a small lithium battery-powered unit. It produces the electrical impulses that start your heartbeat. The generator is implanted under your skin through a small incision. A generator is connected to your heart through tiny wires that are implanted at the same time. The impulses flow through these leads to your heart and are timed to flow at regular intervals just as impulses from your heart's natural pacemaker would.
A pacemaker senses every heartbeat the patient has and only paces the heart when the patient's heart rate falls below a pre-set limit. When the pacemaker works only when it is needed it is called a demand pacemaker. A demand pacemaker has a sensing device that shuts it off if the heart rate is above a certain rate. When the heart is beating slower than the pacemaker rate, the sensing device turns the pacemaker on again. Patients are usually completely unaware of when the pacemaker is pacing their heart.
When is a pacemaker indicated?
A pacemaker is a treatment for a dangerously slow heart rate or arrhythmia. Frequently, pacemakers are necessary following a heart attack or cardiac surgery. Without treatment, a slow or irregular heart rate can lead to weakness, confusion, dizziness, fainting, shortness of breath and even death. Slow heart rates can be the result of metabolic abnormalities or occur as a result of blocked arteries to the heart's conduction system. Slow heart rates can also be a side effect of certain medications.
The sinoatrial node may speed up or slow down the rate at which it sends its electrical impulse. If the sinoatrial node slows down the rate, the heart chambers do not contract often enough to supply the proper amount of blood to your body. This type of arrhythmia is called bradycardia. If the sinoatrial node speeds up the rate, the heart chambers do not have enough time to fill with enough blood to adequately perfuse the body's tissues. This type of arrhythmia is called tachycardia.
Problems may also occur with the electrical pathway between the upper heart (atria) and the lower heart (ventricles). The electrical signals sent out by the sinoatrial node may be delayed in the atrioventricular node (AV node) or may fail to reach the ventricles all together. This arrhythmia is called heart block. Heart block may also cause poor timing with the atria and the ventricles. Doctors call this condition asynchrony. As a result, the ventricles will not fill with enough blood before contracting.
* There are several other arrhythmias that may be treated with a pacemaker. These are only four of the most common reasons why patients need a pacemaker.
What happens during implantation of a pacemaker?
Fortunately, having a pacemaker implanted is only a minor surgical procedure. This is not an open-heart surgery. The procedure is performed with mild sedation and a local anesthetic. Patients are not put to sleep. An area of skin in the upper chest area is shaved, scrubbed, and then cleaned with a special antiseptic. You are given injections of numbing medicine in that area. The doctor may touch the area and ask you when you start to lose sensation in your upper chest.
A small, approximately 2-inch incision is made parallel to and just below the collarbone. A thin flexible wire (called the lead) is inserted into a vein that lies just under the collarbone. The doctor gently advances the lead through that vein under fluoroscopic guidance into the heart. The fluoroscope may be thought of as a kind of moving X-ray picture. Once the lead enters the heart, the doctor attaches it to the tissue inside the heart. At this point, the doctor will test the lead to see if it is in a suitable place for pacing. The testing is not painful. After the lead test, your doctor may decide to move the lead and run the test again. Repositioning and retesting a pacing lead several times is not unusual in pacemaker surgery.
The other end of the pacer wires are connected to a "generator" that is implanted under the skin beneath the collarbone. This generator is about half an inch deep and one and a half inches wide. The skin is then sutured closed and the patient leaves the hospital later that same day or the following day. Pain around the incision is mild and transient and usually responds to Tylenol. It is possible to feel the pacer generator under the skin and a slight deformity of the skin can be visually noticed.
What are possible complications?
Any surgical procedure includes the possibility of complications. The most typical complications for pacemaker implantation are not life threatening, but may require a longer hospital stay or a repeated operation. The most common complications include bleeding, infection, lead dislodgement, and problems with the pacemaker working properly. Ask your doctor about potential complications before your surgery.
Do pacemaker batteries wear out?
The pacemaker contains batteries that will wear down over time, just like any electronic device. The batteries wear down, your pacemaker will slow down, but it will not stop right away. Most batteries last at least 5 years. Using a special analyzer, the doctor can detect the first warning that the batteries are running down. This can be done before you detect any changes yourself. A sudden major slowing down of your heart rate, which you may detect, indicates a more serious problem. If that occurs, call your doctor.
Patient instructions after implantation.
1. SYMPTOMS TO REPORT TO YOUR DOCTOR
- Fever of 100°F or above, and or chills
- Unusual drainage, redness, bleeding, or severe pain around the incision site
- Increased swelling in arm on same side as pacemaker
- Dizziness, faintness, or blacking out
- Pulse less than the pre-set heart rate
2. ACTIVITY
- DO NOT raise affected arm above shoulder level for 48 hours after surgery
- No large arm movements for 1 month (I.e., no golf, tennis, shoveling, etc.)
- Avoid massaging around the area of the pacemaker
- Avoid contact sports that could result in blows to your pacemaker
- If you have steri-strips only, gently wash site with soap and water, pat dry
- You may shower if you have a clear plastic dressing over the steri-strips
3. SPECIAL INSTRUCTIONS
- Inform staff you have a pacemaker before any X-ray, MRI, or scan
- Inform all doctors/dentists you see that you have a pacemaker
- Carry your pacemaker identification card with you at all times
- Wear a medic alert bracelet or necklace
- Keep all follow up appointments with your doctor to insure the pacemaker and battery are functioning properly
- Your pacemaker is sensitive to strong electrical and magnetic fields
- If you use a cellular phone, hold the phone on the opposite ear from the pacemaker / 6 inches away
4. THINGS TO AVOID *Keep the following potential sources of strong electrical or magnetic fields at lease 30 cm (12 inches) away from your Pacemaker.
- Large stereo speakers
- Strong magnets
- Magnetic bingo wands
- Magnetic wands and detectors used in airport security
- Industrial equipment like power generators / arc welders
- Avoid leaning over running engines
- Many amusement park rides have strong magnets and should be avoided.
Where is the test performed?
In the cardiac catherization lab.
How long does this test take?
Typically the procedure takes 1-2 hours to perform
Surgeries
- Abdominal Aortic Aneurysm Repair
- Bypass Surgery
- Carotid Endarterectomy (CEA)
- Coronary Artery Bypass Surgery (CABG)
- Transmyocardial Revascularization (TMR)
- Valve Repair Surgery
- Valve Replacement Surgery
Procedures
- Ablation
- Angiojet Thrombectomy
- Aortagram
- Atherectomy
- Automatic Implantable Cardioverter Defibrillators (AICD or ICD)
- Coil Embolization
- Computed Axial Tomography (CAT or CT)/Ultrafact Computed Tomography (CT) Scan
- Coronary Balloon Angioplasty & Stenting
- Coronary Catheterization
- Dobutamine Stress Echo
- Echocardiography (ECHO)
- Electrocardiogram (EKG/ECG)
- Electrophysiology Study (EPS)
- Event Recorder
- Holter Monitoring
- Inferior Vena Cava (IVC) Umbrella Placement
- Intraaortic Balloon Pump
- Intracardiac Ultrasound (ICE)
- Intravascular Ultrasound (ICE)
- Magnetic Resonance Imaging (MRI)/ Magnetic Resonance Angiography (MRA)
- Medicated Stents
- Nuclear Stress Tests
- Pacemakers
- Percutaneous Transluminal Angioplasty (PTA)
- Percutaneous Transluminal Coronary Angioplasty (PTCA)
- Peripheral Stents
- Peripheral Vascular Angiography
- Radiation Brachytherapy
- Septal Closures
- Signal Averaged Electrocardiogram (SAECG)
- Stents
- Stress Echocardiogram
- Stress Test
- Thrombolytic Treatment
- Tilt Table
- Transesophageal Echocardiogram (TEE)
- Valvuloplasty
